There are a range of substances that can cause serious harm to pets. Listed below are just a few of the common products that you need to prevent your pet gaining access to.
Grapes, sultanas & raisins: The toxic substance in grapes, sultanas and raisins is unknown, however ingestion may cause kidney failure in sensitive pets and there is no ‘safe’ dose.:fill(transparent,1)/raisins3x-56a495555f9b58b7d0d7af32.jpg)
Caffeine: is a stimulant and pets are more sensitive to the effects of caffeine than people. A couple of laps of tea or coffee are unlikely to do any harm, but if your pet swallows a handful of coffee beans, coffee grinds or tea bags they could be in danger.

Chocolate: contains a stimulant called theobromine which is poisonous to pets. The darker the chocolate the more theobromine it contains. Signs of theobromine poisoning include vomiting, diarrhoea, restlessness, hyperactivity and seizures this can lead to cardiac arrest.

Mouldy foods: including bread, nuts and dairy products, contain lots of toxins that could make your pet very ill so keep all pets away from compost.

Onions, garlic, and chives: eating these vegetables and herbs can cause stomach and gut irritation and potentially lead to red blood cell damage and anaemia.

Alcohol: is significantly more toxic to pets than to humans. When consumed, even small quantities of alcoholic beverages and food products may cause vomiting, diarrhoea, decreased coordination, central nervous system depression, difficulty breathing, tremors,
blood changes, coma and death.

Macadamia nuts: within 12 hours of ingestion, macadamia nuts can cause dogs to experience weakness, depression, tremors, vomiting and increased body temperature.

Yeast dough: the rising dough causes gas to accumulate in the pet’s digestive system. Not only can this be painful, but it may also cause the stomach or intestines to become blocked. So while small bits of bread can be given as a treat — never give your pet yeast dough.
/Dough183834031-56a9c28d3df78cf772aa4e3a.jpg)
Bones: dogs regularly present to vets for emergency surgical procedures to remove intestinal obstructions after swallowing pieces of bone that become stuck. Other conditions bones frequently cause include constipation, pancreatitis, teeth fractures as well as internal injury such as bone splinters which can puncture your dog’s digestive tract.

Corn on the cob: if your dog swallows large chunks of the cob, or even the whole cob, it can cause an intestinal blockage due to its size and shape. Signs to look out for are vomiting, loss of appetite or reduced appetite, absence of faeces or diarrhoea and abdominal discomfort.
/corn_fresh-589ea09f3df78c47588d10be.jpg)
Xylitol: is an artificial sweetener found in many products that causes insulin release which can lead to potentially fatal hypoglycaemia (lowered sugar levels).

Milk: feeding your dog milk and other milk-based products can cause diarrhoea or other digestive upsets.

Blue cheese: the roquefortine C found in blue cheese may cause
vomiting and diarrhoea, can lead to tremors, twitching, seizures and
high temperature.

Death cap mushrooms: Are lethal to pets and humans –
no contact is safe.














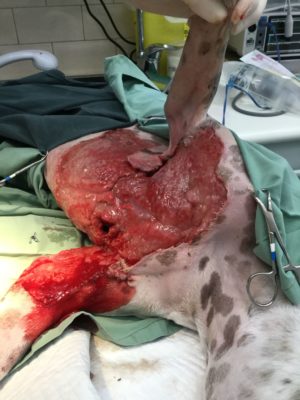 This was the large, open wound left behind after surgically removing all of the dead skin and tissue on Gov'nor's chest.
This was the large, open wound left behind after surgically removing all of the dead skin and tissue on Gov'nor's chest. The colourful bandage vests help to hold his wound dressings in place.
The colourful bandage vests help to hold his wound dressings in place.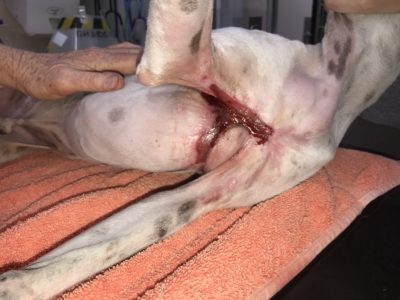 2 months later, Gov'nor is well and truly on his way to feeling like his old self again.
2 months later, Gov'nor is well and truly on his way to feeling like his old self again.

 Variations in colour of the Eastern Brown Snake.
Variations in colour of the Eastern Brown Snake.


 Hall Veterinary Surgery will be closed on the two upcoming ACT public holidays.
Hall Veterinary Surgery will be closed on the two upcoming ACT public holidays.